| AI in Clinical Medicine, ISSN 2819-7437 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, AI Clin Med and Elmer Press Inc |
| Journal website https://aicm.elmerpub.com |
Review
Volume 2, April 2026, e18
Artificial Intelligence Applications in Pediatric Obesity Medicine: Bridging Predictive Analytics, Clinical Decision Support, and Family-Centered Care
Jyothi Ranga Patria, d , Mahika Shettyb, d, Venkata Sushma Chamarthic
aHeritage Valley Family Medicine Residency Program, Beaver Falls, PA, USA
bDrexel University School of Medicine, Philadelphia, PA, USA
cDepartment of Pediatrics, Valley Children’s Healthcare, Madera, CA, USA
dCorresponding Authors: Jyothi Ranga Patri, Heritage Valley Family Medicine Residency Program, Beaver Falls, PA 15010, USA; Mahika Shetty, Drexel University School of Medicine, Philadelphia, PA, USA
Manuscript submitted February 19, 2026, accepted April 3, 2026, published online April 9, 2026
Short title: AI in Pediatric Obesity Medicine
doi: https://doi.org/10.14740/aicm18
| Abstract | ▴Top |
Childhood obesity represents a significant public health challenge, affecting over 340 million children and adolescents worldwide. Despite the implementation of various intervention strategies, prevalence rates continue to rise. Artificial intelligence (AI) technologies offer considerable potential to address this crisis by enhancing risk prediction and individualizing treatment plans through scalable, family-oriented interventions. This review examines current evidence regarding AI applications in pediatric obesity medicine, with a focus on clinical utility, evaluation, and recommendations for future implementation. A comprehensive narrative review of the peer-reviewed literature was conducted to evaluate the applications of AI in pediatric obesity care. The review encompassed predictive analytics, clinical decision support systems (CDSS), remote monitoring technologies, and natural language processing (NLP) tools. PubMed, Scopus, and IEEE databases were systematically searched for studies published between 2015 and 2024 with a focus on validated AI systems with demonstrated clinical applications in pediatric populations. Studies were identified using combinations of keywords including “artificial intelligence,” “machine learning,” “deep learning,” “pediatric obesity,” “clinical decision support,” “predictive analysis,” “telemedicine,” “remote monitoring,” and “natural language processing.” Inclusion criteria included peer-reviewed English-language publications that described AI applications with relevance to pediatric obesity screening, prevention, or management. Studies were excluded if they addressed adult populations exclusively or focused on AI methodology without clinical application. Reference lists of relevant articles were also reviewed to identify additional eligible studies. Two authors (JRP and VSC) independently screened titles and abstracts, with discrepancies resolved through discussion. It is important to note that no AI system is currently approved or used in routine pediatric obesity clinical care; most applications described in this review remain in research or early pilot phases. AI applications demonstrate significant potential in managing various aspects of pediatric obesity. Machine learning algorithms facilitate earlier identification of high-risk children, achieving 75–90% accuracy in predicting obesity risk, as reported in studies employing logistic regression, random forest, and gradient boosting models on longitudinal electronic health record datasets. CDSS can generate effective treatment recommendations tailored to individual metabolic profiles, behavioral patterns, and family circumstances. Remote monitoring platforms that incorporate wearable devices and mobile health applications enable patient engagement and real-time adjustments to interventions. Automated screening and documentation through NLP tools may reduce clinician workload and enhance care quality. However, major implementation challenges include algorithmic bias, data breach risks, limited interoperability, and disparities in patient access to technology. AI applications enhance prediction accuracy, enable personalized interventions, and increase scalability, thereby offering substantial opportunities to advance pediatric obesity care. Key steps for effective integration involve addressing technical challenges, enhancing equity and access, ensuring clinical oversight, and adhering to family-centered care principles. Future research should prioritize improving validation across diverse populations by assessing long-term outcomes and developing implementation frameworks that support, rather than replace, the therapeutic relationship between communities and healthcare providers.
Keywords: Artificial intelligence; Machine learning; Pediatric obesity; Childhood obesity; Predictive analytics; Clinical decision support; Telemedicine; Precision medicine
| Introduction | ▴Top |
Childhood obesity represents a significant public health challenge in the 21st century, affecting an estimated 340 million children and adolescents aged 5 to 19 years worldwide [1]. In the United States, approximately 19.7% of children and adolescents are classified as obese. Studies indicate that this burden is disproportionately higher among racial and ethnic minority groups, as well as among individuals from low-income families [2]. The immediate health consequences of this condition include metabolic syndrome, type 2 diabetes, hypertension, and psychosocial complications. Additionally, it increases the future risk of adult obesity and chronic diseases [3]. Although extensive research and numerous interventions have been developed, traditional pediatric obesity management strategies demonstrate limited long-term effectiveness, typically yielding only modest, unsustained weight outcomes in most behavioral interventions [4].
The etiology of pediatric obesity is multifactorial, encompassing genetic predisposition, metabolic factors, behavioral patterns, family dynamics, environmental influences, and social determinants of health. Consequently, effective management requires sophisticated and personalized approaches that are not attainable through traditional, one-size-fits-all interventions [5]. Furthermore, barriers such as limited access to specialists, insufficient time for comprehensive behavioral assessment and counseling, and difficulties in maintaining long-term engagement with patients and families hinder the provision of intensive, family-centered obesity care [6].
Artificial intelligence (AI) technologies, including machine learning (ML), deep learning, natural language processing (NLP), and predictive analytics, offer significant potential solutions to these challenges [7]. AI systems can process large volumes of heterogeneous data across healthcare systems, including electronic health records (EHRs), genetic information, behavioral patterns, environmental factors, and social determinants. These solutions enable the generation of individualized risk assessments, treatment recommendations, and intervention strategies, thereby facilitating personalized patient management [8]. Furthermore, AI-supported remote monitoring applications and telemedicine platforms can improve access to specialists, thereby reducing the burden on healthcare systems [9].
Despite increased access to and investment in AI within healthcare, studies have demonstrated that the pediatric obesity specialty remains underrepresented in AI research and implementation [9]. Significant progress has been made in AI applications for the management of adult chronic diseases and certain pediatric conditions. However, comprehensive reviews specifically addressing AI in pediatric medicine are lacking. Pediatric obesity management differs from adult medicine due to unique developmental, familial, and ethical considerations, making this gap particularly concerning. Unique pediatric considerations include the influence of growth and pubertal development on body composition trajectories, the central role of families and caregivers in behavioral interventions, age-dependent metabolic variability, and stricter ethical and privacy regulations governing the use of minor’s health data [10].
This review synthesizes current evidence regarding AI applications in pediatric obesity management across four primary domains: predictive analytics and risk stratification, clinical decision support systems (CDSS), digital medicine and remote monitoring technologies, and NLP integrated with EHRs. The evidence supporting each domain is examined with careful attention to implementation strategies, particularly regarding algorithmic bias and equitable access. This analysis aims to identify critical gaps and challenges while providing a comprehensive understanding of potential AI technologies to improve pediatric obesity care, and to offer recommendations for pediatricians, obesity medicine specialists, family physicians, and other healthcare professionals.
| Predictive Analytics and Risk Stratification | ▴Top |
Early identification of high-risk individuals within periodic population screenings for obesity provides a critical opportunity for timely intervention and prevention. However, the predictive accuracy of traditional risk assessment methodologies remains limited. ML algorithms have demonstrated promise for predicting obesity risk in adult populations and are currently under investigation for pediatric applications [9]. These approaches leverage data extracted from EHRs and incorporate diverse sources, including biometric parameters, early childhood growth patterns, parental characteristics, socioeconomic status, and environmental variables. It is important to note that much of the available evidence derives from adult or general medical populations, and its direct applicability to pediatric obesity must be interpreted with caution; studies specific to pediatric cohorts remain limited.
Research demonstrates that ML applications achieve superior predictive performance compared to traditional statistical methods across various healthcare platforms [10]. These algorithms facilitate the identification of high-risk children by analyzing growth trajectories, family history, and early-life risk factors in childhood obesity research [11]. Such models enable more effective predictions when additional variables, including birth weight, parental obesity status, and social determinants of health, are incorporated.
AI applications, including deep learning models, can analyze complex nonlinear relationships and process high-dimensional data. Using convolutional neural networks and other advanced architectures, it is possible to identify critical inflection points in pediatric EHR growth patterns that precede clinical obesity diagnosis through longitudinal growth trajectory analysis. This capability enables the timely identification of intervention windows for the development of preventive strategies [12].
ML applications can support population-level risk stratification in addition to individual-level predictions. These approaches facilitate targeted allocation of limited prevention and treatment resources for obesity prevention. An optimal stratification system can use EHR data to categorize children into low, moderate, and high-risk groups. This methodology enables intentional prioritization of intensive behavioral interventions for high-risk categories, while low-risk children can be directed to traditional universal prevention programs [5].
Despite advancements in AI applications, significant barriers remain in translating clinical data using predictive models. Many algorithms demonstrate limited accuracy in identifying racial and ethnic minority populations, as well as children from low-income families, who are disproportionately affected by obesity [13]. This algorithmic bias often arises from training datasets that do not adequately represent diverse populations or from a failure to effectively account for social determinants of health and structural inequities [14]. Healthcare providers may be reluctant to use these data when predictions are not reproducible, and the interpretability of ML models undermines clinical trust [15].
| CDSS | ▴Top |
CDSS are AI applications that analyze patient-specific data to generate personalized recommendations, thereby assisting healthcare providers in making evidence-based treatment decisions [16]. These systems have demonstrated significant potential in addressing the complex and heterogeneous nature of pediatric obesity care, which often limits the effectiveness of conventional treatment protocols [17].
AI-powered CDSS are being developed to personalize obesity treatment recommendations. These technologies integrate factors such as individual metabolic phenotypes, behavioral patterns, and psychosocial variables into the design of intervention strategies. Such applications analyze EHR data for family dietary and physical activity patterns, and psychosocial assessments to generate individualized care plans. These plans are typically aligned with evidence-based guidelines and aim to address family-specific barriers to effective obesity care [18]. Early implementation in pediatric primary care settings has the potential to enhance adherence to comprehensive obesity assessment and counseling practices.
Studies indicate that ML applications can facilitate the identification of treatment-responsive phenotypes, potentially enabling early prediction of interventions that may benefit individual patients. These models can also predict responses to various obesity treatment modalities, including dietary interventions, physical activity promotion, and comprehensive behavioral therapy. Treatment outcomes generally depend on characteristics such as age, metabolic parameters, family structure, and readiness for behavioral modifications [8]. As seen in Table 1, ML further helps efficiently match patients to appropriate interventions in line with established guidelines [11, 12, 16–20].
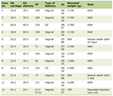 Click to view | Table 1. Current Artificial Intelligence Applications in Pediatric Obesity Medicine by Domain and Technology Category |
Reinforcement learning algorithms are being USED for personalizing the intensity and modality of obesity treatment over time by learning optimal decision-making through trial-and-error interactions with dynamic environments. These systems can make real-time adjustments to recommendations and optimize intervention dosages based on individual treatment responses, thereby reducing financial burdens for families [12]. However, the validation of these approaches remains limited in real-time applications.
Despite the demonstrated potential of CDSS, several barriers hinder their implementation. Integrating these models with existing EHR systems necessitates substantial technical infrastructure and workflow redesign. Additional challenges include healthcare providers’ concerns about liability, the preservation of clinical autonomy, the reliability of AI-generated recommendations, and the time required to review and implement CDSS outputs [16]. Furthermore, it is essential to uphold family-centered principles and ensure that recommendations are consistent with family preferences and cultural values.
| Telemedicine and Remote Monitoring Technologies | ▴Top |
The COVID-19 pandemic led to a rapid increase in the adoption of telemedicine for patient care, including obesity management, and highlighted both the opportunities and limitations of virtual healthcare delivery [21]. Remote monitoring technologies and telemedicine platforms enhanced by AI have the potential to improve access to obesity management specialists, particularly for underserved populations, and to facilitate more frequent interactions between traditional clinical encounters.
Wearable devices and smartphone applications use AI algorithms to continuously monitor physiological parameters, including physical activity, dietary intake, sleep patterns, and heart rate. These parameters provide real-time insights into behavioral trends and inform adaptive interventions, allowing for early identification of unhealthy behaviors or physiological deviations [18]. Mobile health applications analyze accelerometer data, food images, and self-reported information about food and activity, and deliver personalized prompts to support behavioral modification and motivation. Studies indicate that such real-time interventions may improve physical activity levels and dietary quality among adolescents with obesity.
Computer vision and image recognition algorithms support the development of automated dietary assessment tools and reduce the burden of manual food logging, thereby improving accuracy [19]. These applications enable healthcare providers to continuously monitor dietary patterns by analyzing meal photographs to estimate portion sizes and nutritional content, and to provide real-time feedback to patients and families. Integration of these applications with telehealth platforms facilitates synchronous dietary counseling and supports timely dietary interventions.
Virtual reality and gamification strategies combined with AI-driven personalized algorithms have the potential to enhance engagement, physical activity, and nutrition awareness. These platforms deliver content tailored to individual progress and preferences, utilizing real-time adjustments to difficulty levels and reward systems. This approach may promote behavioral change through dynamic, individualized content delivery [22].
Limitations to the use of AI in pediatric obesity management are diverse. The implementation of remote monitoring technologies is associated with significant inequities in access. Disparities in the availability of smartphones, wearable devices, and reliable internet connectivity exacerbate existing health inequities. Security concerns are particularly critical in pediatric populations and necessitate robust safeguards to prevent data breaches and misuse [23]. Furthermore, excessive screen time and technology-mediated care may undermine social connections and the principles of family-centered care, both of which are essential for effective pediatric obesity treatment.
| NLP and EHR Integration | ▴Top |
NLP is a branch of AI that enables computers to interpret and generate human language. NLP has several practical applications in pediatric obesity management, such as automated screening and identification of pediatric obesity cases, clinical documentation support, and extraction of insights from unstructured clinical notes [20].
NLP algorithms can analyze free-text clinical notes to identify pediatric patients with obesity or related comorbidities that are not typically captured by structured diagnostic ICD codes. This approach addresses underdiagnosis and enhances case ascertainment. Studies from other clinical domains have demonstrated that NLP systems achieve high sensitivity and specificity in identifying pediatric obesity cases from clinical notes, surpassing identification rates based on diagnosis codes [20]. Improved case identification enables more comprehensive population health management and supports quality improvement initiatives in pediatric obesity care.
AI-driven documentation tools that utilize NLP and speech recognition have been shown to reduce physician burnout associated with clinical documentation, particularly during extensive obesity-focused visits. Consequently, these tools increase the amount of time providers can dedicate to direct patient care and family engagement, thereby enhancing patient satisfaction and outcomes. These technologies are also capable of generating patient visit summaries, extracting data relevant to obesity registries, and automatically translating this information into quality measure initiatives [20]. Preliminary evidence from general pediatric care indicates that NLP-supported documentation improves the comprehensiveness of clinical records and reduces providers’ administrative burden [20].
NLP systems facilitate the analysis of clinical narratives to identify patterns, statement strategies, and outcomes that may not be evident in structured data. The analytical capabilities of NLP support quality improvement initiatives, enhance comparative effectiveness research, and help identify best practices in real-world obesity care delivery [9]. Furthermore, NLP can extract data from clinical notes regarding social determinants of health, thereby enabling more comprehensive risk assessments and the development of personalized interventions.
The effective implementation of NLP technologies presents significant challenges. Clinical documentation practices and EHRs exhibit considerable variability, and the complexity of abbreviations and medical jargon requires careful attention to accuracy across diverse linguistic and cultural contexts [19]. Erroneous NLP-generated documentation or case identification may have substantial consequences for patient care, underscoring the need for ongoing scientific validation and concurrent human oversight. The integrated AI workflow in pediatric obesity care is illustrated in Figure 1.
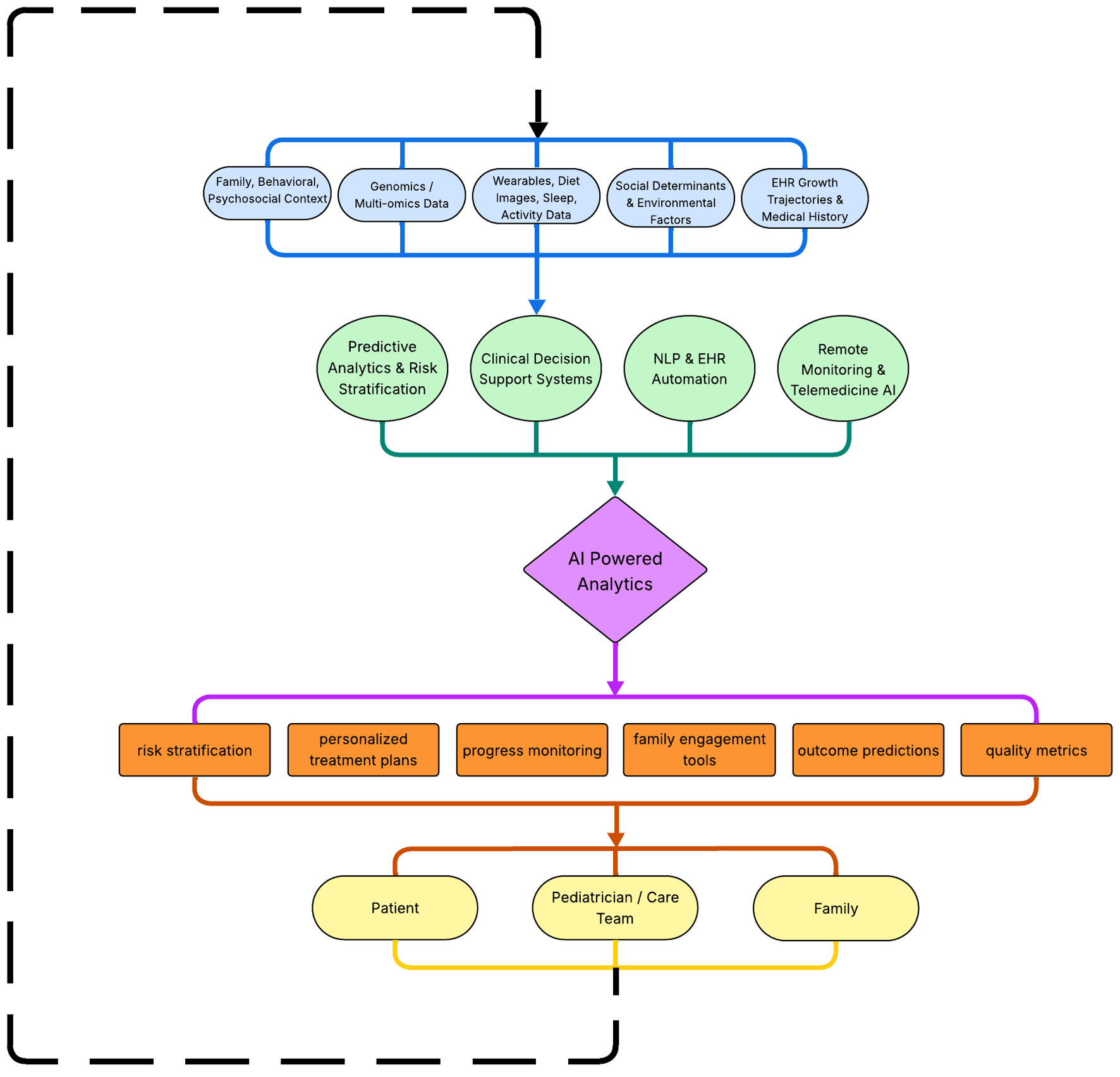 Click for large image | Figure 1. AI workflow in pediatric obesity care pathway. The figure depicts the flow of various information types (e.g. medical records, wearable device data, family context, and environmental factors) into a single AI engine. This engine analyzes the aggregated data and provides insights and guidance to families, patients, and pediatric care teams. Actions taken by these groups generate new data, which are subsequently reintegrated into the AI engine, establishing a continuous feedback loop. Source: Figure created by authors JP, MS, and VSC using Microsoft PowerPoint from data extracted from sources [16–20]. AI: artificial intelligence. |
| Implementation Challenges and Ethical Considerations | ▴Top |
The integration of AI technology into pediatric obesity management presents significant technical, clinical, and ethical challenges [21]. AI systems trained on non-representative datasets may perpetuate and exacerbate health disparities, raising substantial concerns regarding algorithmic bias [13]. Intentional and systematic inclusion of representative and accurate data, along with comprehensive fairness testing, is necessary to achieve equitable performance across diverse populations [22, 23].
Maintaining data privacy and security is particularly important in pediatric populations, given enhanced protections for minors and parental authority over children’s health information. Compliance with regulatory requirements and maintaining family trust are essential for implementing AI systems that process sensitive health data [22]. Table 2 displays how clear communication about data use, storage, and sharing practices is critical for obtaining informed consent and addressing ethical challenges in AI implementation [21–23].
 Click to view | Table 2. Implementation Barriers and Proposed Solutions for AI Integration in Pediatric Obesity Care |
Adapting AI models to ensure interpretability and explainability is essential for fostering clinical trust. Healthcare providers must understand the rationale behind AI-generated recommendations and assess their sustainability to effectively communicate these insights to families, thereby upholding accountability in clinical scenarios [14]. AI platforms should generate predictions with transparent explanations to reduce resistance from both clinicians and families [24–26].
Integrating AI tools into existing clinical workflows and EHR systems presents several practical challenges. AI tools that do not require additional time or effort from clinicians are more likely to be adopted in the long term, regardless of technical sophistication [27]. Research indicates that successful AI integration must address not only algorithmic fairness but also equitable access to AI-enabled technologies and services. Effective implementation depends on user-friendly design, optimized workflows, and adequate training support. Attention to digital literacy, technology access, and the development of culturally appropriate tools that integrate with community-based resources is also necessary. These measures help ensure that AI innovations benefit, rather than marginalize, vulnerable populations [28].
Maintaining a central framework of family-centered care and therapeutic social connections remains essential [29]. AI should support human relationships, clinical judgment, and family empowerment, all of which are fundamental to effective pediatric obesity care. Ongoing evaluation and future research are required to balance technological innovation with holistic, human-centered medical practice.
| Future Directions | ▴Top |
AI research and implementation in pediatric obesity medicine present several promising directions. AI tools must be developed and validated to address the needs of diverse pediatric populations, including various age groups, racial and ethnic backgrounds, and socioeconomic contexts [28]. Future research should prioritize the design of prospective clinical trials comparing AI-enhanced care to standard care, using long-term outcomes such as body mass index (BMI) trends, metabolic health, and psychosocial well-being as critical evidence of AI’s clinical effectiveness.
AI-driven precision medicine approaches can facilitate the identification of novel obesity phenotypes and therapeutic targets by integrating multi-omics data, such as genomics, metabolomics, and microbiome analysis, with clinical, behavioral, and environmental information systems [30]. These strategies, in turn, support the development of personalized treatment plans that target specific biological mechanisms underlying obesity.
Future research should also explore the development of federated learning approaches, which enable the training of AI models across multiple institutions without sharing sensitive patient data. This strategy addresses privacy concerns while enabling the creation of robust models from large, diverse datasets [31]. The expansion of such methodologies, where data remain distributed across various healthcare systems, is particularly valuable for pediatric populations by enhancing data security.
Research into AI applications that primarily focus on obesity prevention, rather than treatment, represents an underexplored opportunity [32]. As seen in Figure 2, this approach may lead to the development of more effective and cost-efficient strategies, as AI-powered early intervention systems can identify and support families during critical developmental periods such as pregnancy, early childhood, and adolescence.
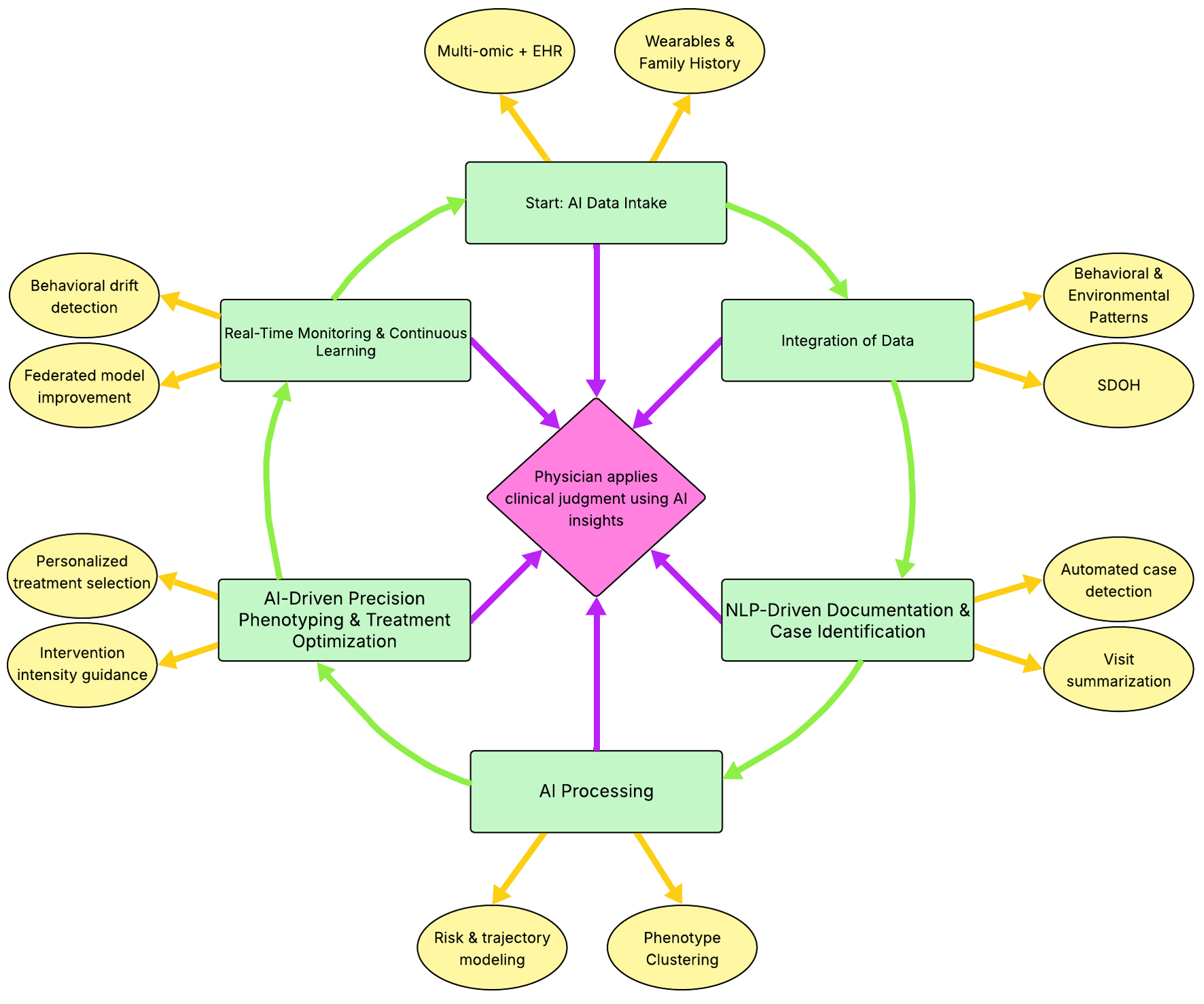 Click for large image | Figure 2. Future integration model for AI in precision pediatric obesity medicine. This model illustrates a continuous learning system that integrates multi-omic, clinical, behavioral, environmental, and social determinants data to inform individualized obesity management. Following data intake and contextual integration, AI processing supports risk modeling, growth trajectory analysis, and phenotype clustering to guide precision phenotyping and treatment optimization. NLP-enabled documentation facilitates case identification and reduces clinical documentation burden. Real-time monitoring enables adaptive intervention adjustments and ongoing model refinement. Clinical decisions remain physician-led, with AI providing structured insights to support personalized treatment selection and longitudinal response assessment. Source: Figure created by authors JP, MS, and VSC using Microsoft PowerPoint from data extracted from sources [28–30]. AI: artificial intelligence; NLP: natural language processing. |
| Conclusions | ▴Top |
AI shows emerging potential to support pediatric obesity care by enabling improved risk assessment, individualized clinical decision-making, scalable remote monitoring, and optimized AI-driven health records. ML algorithms have shown promise in identifying children at elevated risk for obesity, while CDSS provide tailored treatment recommendations. Remote monitoring platforms facilitate sustained patient engagement, and NLP tools improve case identification and documentation.
However, achieving these benefits necessitates addressing challenges, including algorithmic bias, data privacy and security concerns, limited interoperability, implementation barriers, and health inequities. Effective integration requires rigorous validation across diverse populations, user-centered design aligned with clinical workflows, and robust privacy protections with transparent algorithms. Collaboration among pediatric providers, obesity specialists, researchers, and policymakers is crucial to ensure that AI augments clinical judgment and therapeutic relationships. With thorough evaluation, AI can enhance prevention and treatment efforts, broaden access, and improve outcomes for children globally. While most applications remain in research or early pilot phases, continued development and rigorous clinical validation are essential.
Acknowledgments
None to declare.
Financial Disclosure
None to declare.
Conflict of Interest
The authors declare no conflict of interest related to this manuscript.
Author Contributions
JP contributed to the conceptualization, literature review, manuscript drafting, and critical revision. MS assisted with formatting and developed flowcharts, including interpretation of data from the literature, and revising the manuscript. VSC was responsible for conceptualization, literature review, manuscript drafting, and critical revision. All authors approved the final manuscript.
Data Availability
This review article is based exclusively on published literature. No original data were generated. All cited references are accessible through their respective publishers.
Abbreviations
AI: artificial intelligence; BMI: body mass index; CDSS: Clinical Decision Support Systems; EHR: electronic health record; ML: machine learning; NLP: natural language processing
| References | ▴Top |
- World Health Organization. Obesity and Overweight [Internet]. World Health Organization. 2025. Available from: https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight.
- Fryar CD, Carroll MD, Afful J. Prevalence of overweight, obesity, and severe obesity among children and adolescents aged 2-19 years: United States, 1963-1965 through 2017-2018. NCHS Health E-Stats. 2020.
- Kumar S, Kelly AS. Review of childhood obesity: from epidemiology, etiology, and comorbidities to clinical assessment and treatment. Mayo Clin Proc. 2017;92(2):251-265.
doi pubmed - Force USPST, Grossman DC, Bibbins-Domingo K, Curry SJ, Barry MJ, Davidson KW, Doubeni CA, et al. Screening for obesity in children and adolescents: US preventive services task force recommendation statement. JAMA. 2017;317(23):2417-2426.
doi pubmed - Skelton JA, Irby MB, Grzywacz JG, Miller G. Etiologies of obesity in children: nature and nurture. Pediatr Clin North Am. 2011;58(6):1333-1354, ix.
doi pubmed - Taveras EM, Gillman MW, Kleinman KP, Rich-Edwards JW, Rifas-Shiman SL. Reducing racial/ethnic disparities in childhood obesity: the role of early life risk factors. JAMA Pediatr. 2013;167(8):731-738.
doi pubmed - Topol EJ. High-performance medicine: the convergence of human and artificial intelligence. Nat Med. 2019;25(1):44-56.
doi pubmed - Yu KH, Beam AL, Kohane IS. Artificial intelligence in healthcare. Nat Biomed Eng. 2018;2(10):719-731.
doi pubmed - Rajkomar A, Dean J, Kohane I. Machine learning in medicine. N Engl J Med. 2019;380(14):1347-1358.
doi pubmed - Winkelman J, Nguyen D, vanSonnenberg E, Kirk A, Lieberman S. Artificial Intelligence (AI) in pediatric endocrinology. J Pediatr Endocrinol Metab. 2023;36(10):903-908.
doi pubmed - Ward ZJ, Long MW, Resch SC, Giles CM, Cradock AL, Gortmaker SL. Simulation of Growth Trajectories of Childhood Obesity into Adulthood. N Engl J Med. 2017;377(22):2145-2153.
doi pubmed - Esteva A, Robicquet A, Ramsundar B, Kuleshov V, DePristo M, Chou K, Cui C, et al. A guide to deep learning in healthcare. Nat Med. 2019;25(1):24-29.
doi pubmed - Obermeyer Z, Powers B, Vogeli C, Mullainathan S. Dissecting racial bias in an algorithm used to manage the health of populations. Science. 2019;366(6464):447-453.
doi pubmed - Gianfrancesco MA, Tamang S, Yazdany J, Schmajuk G. Potential biases in machine learning algorithms using electronic health record data. JAMA Intern Med. 2018;178(11):1544-1547.
doi pubmed - Rudin C. Stop explaining black box machine learning models for high stakes decisions and use interpretable models instead. Nat Mach Intell. 2019;1(5):206-215.
doi pubmed - Sutton RT, Pincock D, Baumgart DC, Sadowski DC, Fedorak RN, Kroeker KI. An overview of clinical decision support systems: benefits, risks, and strategies for success. NPJ Digit Med. 2020;3:17.
doi pubmed - Barlow SE, Expert C. Expert committee recommendations regarding the prevention, assessment, and treatment of child and adolescent overweight and obesity: summary report. Pediatrics. 2007;120(Suppl 4):S164-192.
doi pubmed - Nahum-Shani I, Smith SN, Spring BJ, Collins LM, Witkiewitz K, Tewari A, Murphy SA. Just-in-Time Adaptive Interventions (JITAIs) in mobile health: key components and design principles for ongoing health behavior support. Ann Behav Med. 2018;52(6):446-462.
doi pubmed - Boushey CJ, Spoden M, Zhu FM, Delp EJ, Kerr DA. New mobile methods for dietary assessment: review of image-assisted and image-based dietary assessment methods. Proc Nutr Soc. 2017;76(3):283-294.
doi pubmed - Kreimeyer K, Foster M, Pandey A, Arya N, Halford G, Jones SF, Forshee R, et al. Natural language processing systems for capturing and standardizing unstructured clinical information: A systematic review. J Biomed Inform. 2017;73:14-29.
doi pubmed - Kruse CS, Krowski N, Rodriguez B, Tran L, Vela J, Brooks M. Telehealth and patient satisfaction: a systematic review and narrative analysis. BMJ Open. 2017;7(8):e016242.
doi pubmed - Stephenson A, McDonough SM, Murphy MH, Nugent CD, Mair JL. Using computer, mobile and wearable technology enhanced interventions to reduce sedentary behaviour: a systematic review and meta-analysis. Int J Behav Nutr Phys Act. 2017;14(1):105.
doi pubmed - Price WN, 2nd, Cohen IG. Privacy in the age of medical big data. Nat Med. 2019;25(1):37-43.
doi pubmed - Char DS, Shah NH, Magnus D. Implementing machine learning in health care - addressing ethical challenges. N Engl J Med. 2018;378(11):981-983.
doi pubmed - Rajkomar A, Hardt M, Howell MD, Corrado G, Chin MH. Ensuring fairness in machine learning to advance health equity. Ann Intern Med. 2018;169(12):866-872.
doi pubmed - Vyas DA, Eisenstein LG, Jones DS. Hidden in Plain Sight - Reconsidering the Use of Race Correction in Clinical Algorithms. N Engl J Med. 2020;383(9):874-882.
doi pubmed - Kelly CJ, Karthikesalingam A, Suleyman M, Corrado G, King D. Key challenges for delivering clinical impact with artificial intelligence. BMC Med. 2019;17(1):195.
doi pubmed - Chen IY, Pierson E, Rose S, Joshi S, Ferryman K, Ghassemi M. Ethical machine learning in healthcare. Annu Rev Biomed Data Sci. 2021;4:123-144.
doi pubmed - Verghese A, Shah NH, Harrington RA. What this computer needs is a physician: humanism and artificial intelligence. JAMA. 2018;319(1):19-20.
doi pubmed - Hasin Y, Seldin M, Lusis A. Multi-omics approaches to disease. Genome Biol. 2017;18(1):83.
doi pubmed - Rieke N, Hancox J, Li W, Milletari F, Roth HR, Albarqouni S, Bakas S, et al. The future of digital health with federated learning. NPJ Digit Med. 2020;3:119.
doi pubmed - Bleich SN, Vercammen KA, Zatz LY, Frelier JM, Ebbeling CB, Peeters A. Interventions to prevent global childhood overweight and obesity: a systematic review. Lancet Diabetes Endocrinol. 2018;6(4):332-346.
doi pubmed
This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (CC BY 4.0), which permits unrestricted use, distribution, and reproduction in any medium, including commercial use, provided the original work is properly cited.
AI in Clinical Medicine is published by Elmer Press Inc.