Integrating Artificial Intelligence Into Sepsis Care: A Narrative Review of Predictive Models and Implementation Pathways
DOI:
https://doi.org/10.14740/aicm21Keywords:
Artificial intelligence, Health services, Intensive care, Predictive models, SepsisAbstract
Background: Sepsis is a leading cause of morbidity and mortality, particularly in intensive care units (ICUs). Traditional prediction tools such as systemic inflammatory response syndrome (SIRS), Sequential Organ Failure Assessment (SOFA), and Acute Physiology and Chronic Health Evaluation II (APACHE II) are widely used but have limited specificity, responsiveness, and adaptability. This review evaluates artificial intelligence (AI)-based sepsis prediction models compared with conventional approaches, focusing on predictive performance, clinical integration, and future implementation pathways.
Methods: This narrative review was conducted using a structured literature search of PubMed, Scopus, and Web of Science databases for studies published between 2015 and 2025. Inclusion criteria comprised studies evaluating AI-based sepsis prediction models with reported performance metrics in adult or ICU settings. Approximately 40–50 studies were included after screening titles, abstracts, and references. Data were synthesized qualitatively with emphasis on model performance, validation, and clinical applicability.
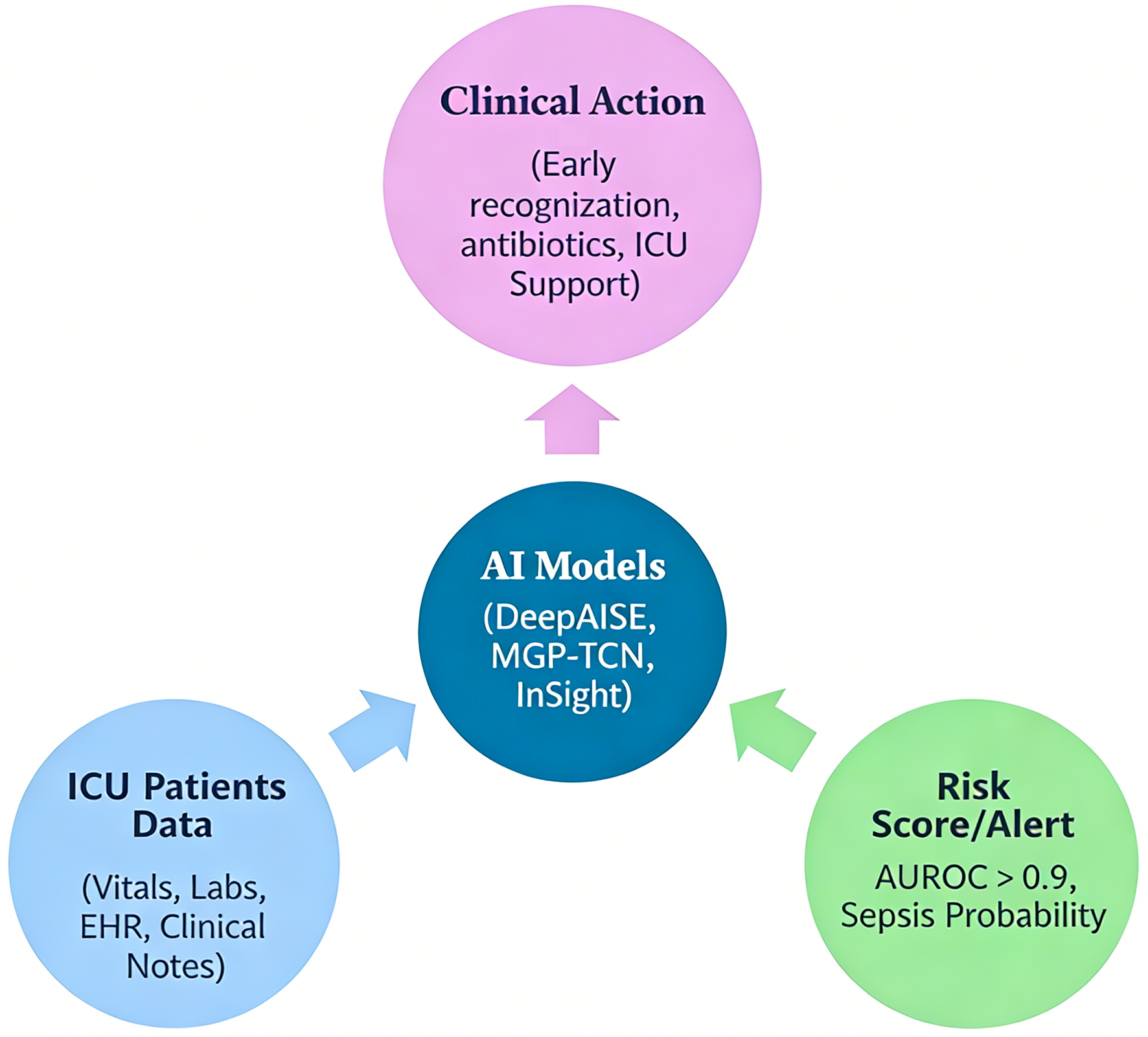
Results: AI-based models generally outperformed traditional tools, with random forest, InSight, and DeepAISE achieving area under the receiver operating characteristic curve (AUROC) values above 0.90, superior sensitivity, and greater adaptability in dynamic ICU environments. Targeted Real-time Early Warning System (TREWS) demonstrated improved patient outcomes in prospective multi-site trials, enabling earlier antibiotic administration by several hours and associated reductions in mortality, highlighting meaningful real-world clinical benefit. Models such as Multi-task Gaussian Process Temporal Convolutional Network (MGP-TCN) further enhanced predictive accuracy using temporal data but remain computationally intensive. Integration into electronic health records and the potential for explainable AI were highlighted as key facilitators for clinical adoption.
Conclusions: AI-driven sepsis prediction models show significant advantages over conventional scoring systems, offering improved accuracy, adaptability, and workflow integration. However, widespread adoption requires multicenter prospective validation, enhanced interpretability to build clinician trust, and supportive policy frameworks to ensure safe, equitable, and sustainable implementation in clinical practice.
Published
Issue
Section
License
Copyright (c) 2026 The authors

This work is licensed under a Creative Commons Attribution 4.0 International License.






